Objective: Eustachian tube dysfunction is known to play an influential role in causing middle ear diseases, which are often connected with nasal and sinusal disorders. Patients with severe symptoms may become resistant to medical treatment and surgical tubodilation. An innovative shockwave tubodilation technique was applied to patients with Eustachian tube dysfunction in this study. It has recently been demonstrated that shockwave tubodilation technique can be successfully applied to the tube level in urology. It has now been positioned at the coronary level, where it has been safely deployed. We believe this is the first study of its kind to demonstrate shockwaves in the Eustachian tube. This technique is based on the belief that shockwaves play an instrumental role in wound healing by regulating macrophages. The immunomodulation achieved by shockwaves may be underestimated as a benefit of clinical applications, which may be applicable to other macrophage-associated diseases. Accordingly, we hypothesized that shockwave tubodilation technique might be effective in treating Eustachian tube dysfunction through immunomodulation. This study aimed to evaluate the effectiveness of shockwave tubodilation in patients with Eustachian tube dysfunction.
Methods: Between November 2020 and February 2021, our study recruited 10 patients who displayed symptoms related to Eustachian tube dysfunction and then underwent shockwave tubodilation therapy. Patients received regular otolaryngological visits with audiological examinations. Our investigation consisted of the following procedures: an audiometric and impedance examination, rhinomanometry, otovideoendoscopy, the Italian nose obstruction symptom evaluation (I-NOSE) scale, the Sino-Nasal Outcome Test-22 (SNOT-22) questionnaire, and the Eustachian Tube Dysfunction Questionnaire-7 (ETDQ-7). Postoperative examinations and specialist examinations were performed for the patients after 2 weeks and 4 weeks following the procedure.
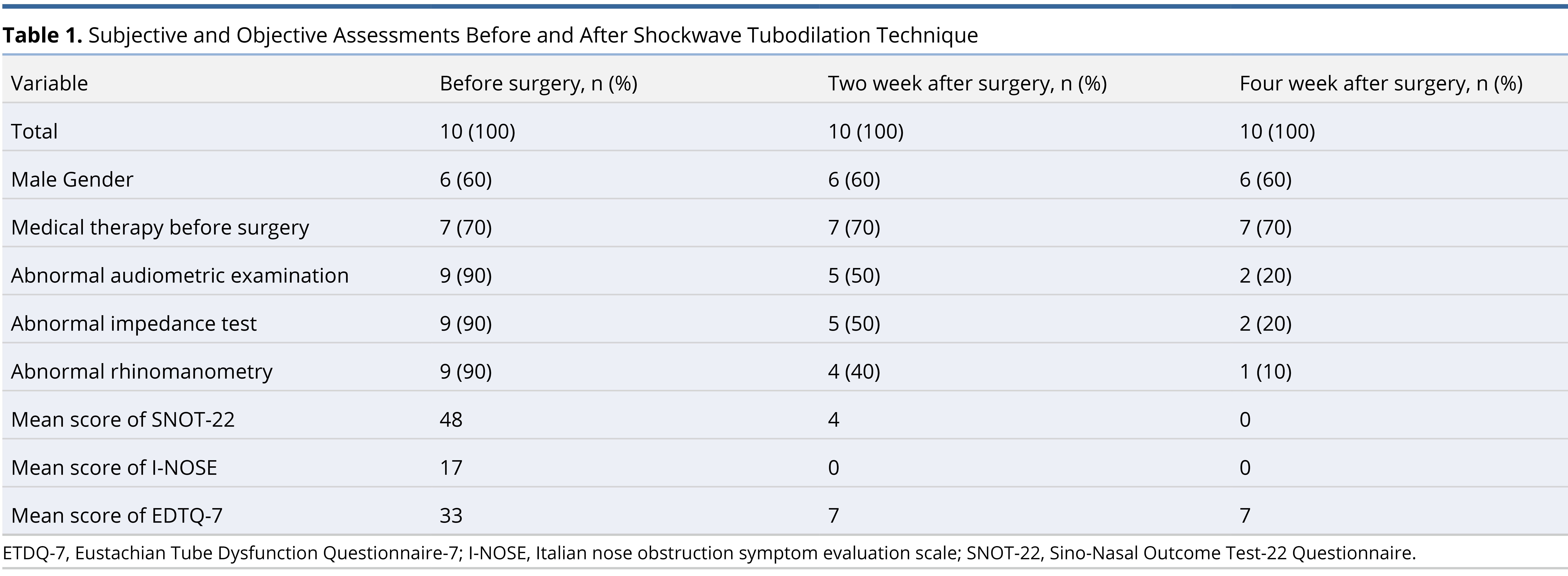
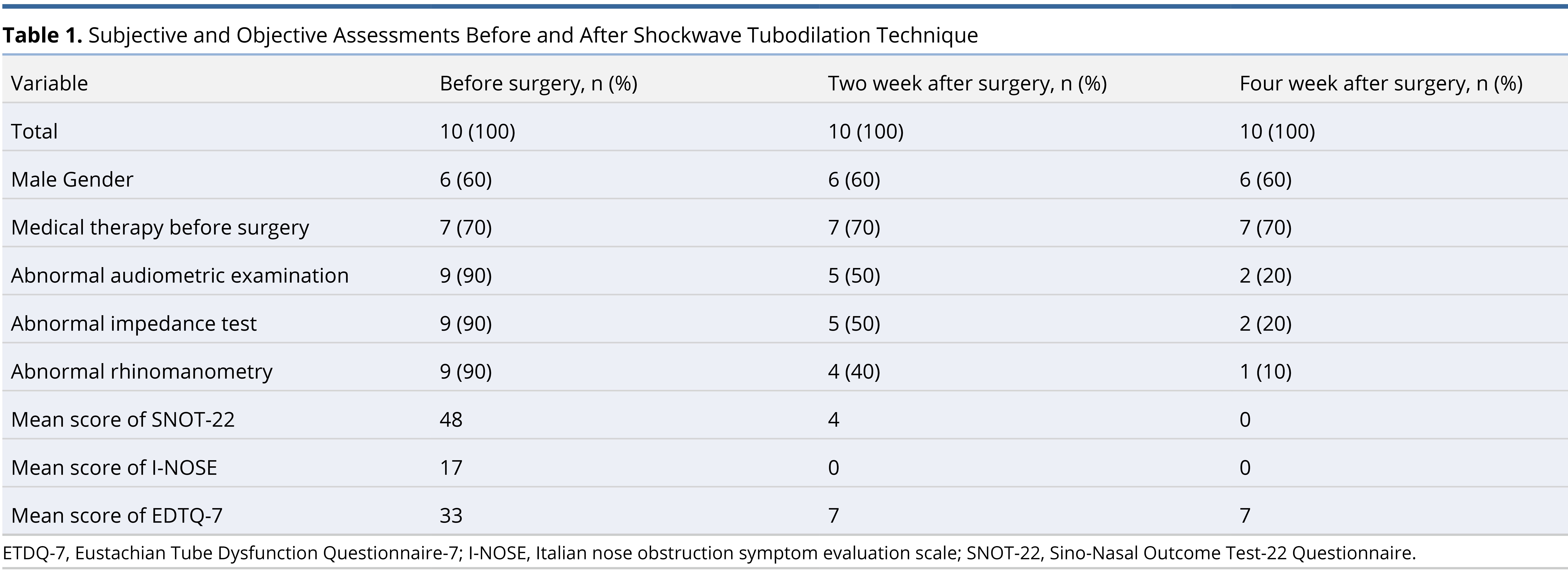
Results: The patients enrolled in the study ranged in age from 35 to 70 years old. Before surgery, 9 out of 10 patients (90%) had abnormal results on the audiometer, but only 5 out of 10 (50%) had abnormal results 2 weeks after surgery, and 2 out of 10 (20%) had abnormal results 4 weeks after surgery. Nine patients (90%) had abnormal impedance test results before surgery, but only 5 (50%) patients after surgery, and 2 (20%) patients 4 weeks after surgery. The rhinomanometer results were abnormal in 9 out of 10 cases (90%) prior to surgery, but only 4 of 10 patients (40%) had abnormal results 2 weeks following surgery, and only one patient (10%) had abnormal results 4 weeks after surgery. Based on the results of the responses to the SNOT-22, I-Nose, and ETDQ-7 questionnaires, patients who had undergone shockwave tubodilation therapy showed an improvement. There were no complications observed.
Conclusion: Based on subjective and objective assessments, shockwave tubodilation has been demonstrated to be effective in treating patients suffering from Eustachian tube dysfunction. The preliminary results have provided the impetus for us to continue our research and expand the number of cases studied to determine if the positive short-term outcomes of shockwave tubodilation have led to permanent improvement.
A Eustachian tube consists of an osseous posterolateral portion and a fibrocartilaginous anteromedial portion. An osseous portion is made up of the petrous part of the temporal bone, while a flexible portion is made up of the tubal cartilage and its surrounding tissue. The fibrocartilaginous portion plays the main role in the active function of the tube. Through suspensory ligaments, the fibrocartilaginous portion is connected to the skull base. In relation to the mediosagittal plane and to the horizontal plane, the longitudinal axis of the tube forms an angle. Adults have an angle of 45 degrees between the longitudinal axis of the cartilaginous part of the Eustachian tube and the mediosagittal plane, while infants have an angle of about 10 degrees. Adults usually have an average angle of 35 degrees between the Frankfurt horizontal plane (orbitomeatal plane) and the tubal longitudinal axis. Eustachian tubes range in length from 31 to 44 cm in adults but are only about half that length in newborns [1,2].
Several anatomic studies have been conducted concerning the Eustachian tube, however these were histopathologic studies performed on cadavers, making it difficult to correlate the findings with clinical circumstances [3-6]. Additionally, only a small number of subjects were included in these studies. With the use of the multiplanar reformation technique on computed tomography, it was found that patients with a stenotic Eustachian tube had a small bony framework, particularly near the isthmus, and a thick soft tissue lining, particularly near the tympanic cavity. The condition was considered to be one of the possible causes of tubal stenosis. These findings may prove helpful in identifying and managing Eustachian tube disorders [7].
Eustachian tube dysfunction is common among US adults; it is estimated that 4.6% of adults have Eustachian tube dysfunction, which rises to 48.5% when examined by questionnaire among patients with chronic rhinosinusitis [8]. Chronic sinonasal inflammation may lead to a dysfunctional Eustachian tube, which may then result in middle ear diseases [2,9]. Eustachian tube dysfunction is characterized by auricular fullness, hearing impairment, intermittent tinnitus, and a feeling of imbalance.
Eustachian tube balloon dilation, developed by Sudhoff [10,11], offers a minimally invasive treatment option for Eustachian tube dysfunction. During this procedure, an inflatable balloon catheter is inserted through the nasopharyngeal ostium into the Eustachian tube under an endoscopic view. The balloon catheter is then filled with saline to a pressure of ten bars and positioned for two minutes in the Eustachian tube. Following this step, the catheter is deflated and removed [12-14]. Our substantial experience in treating Eustachian tube dysfunction led us to develop a novel combined approach to Eustachian tube dysfunction using minimally invasive devices. It was found that the combined procedure is an effective, safe, and comprehensive treatment for tubal dysfunction in patients [9].
Research has shown that shock waves are key regulators of macrophage functions related to wound healing. This immunomodulatory effect may also apply to other diseases in which macrophages are involved, such as disorders of the Eustachian tube [15,16]. Based on this concept, we developed a novel shockwave tubodilation technique for patients with Eustachian tube dysfunction. We conducted a preliminary study to determine the feasibility and effectiveness of shockwave tubodilation technique in treating stenotic Eustachian tube dysfunction.
Between November 2020 and February 2021, we retrospectively enrolled 10 patients with refractory otitis media with effusion related to Eustachian tube dysfunction. It was reported that all the patients presented with rhinosinusitis as well as severe aural fullness and compensatory difficulties, which had failed to be resolved by medical treatment for five months. Decongestant and antihistamine nasal sprays were administered as part of the treatment for chronic rhinitis and associated Eustachian tube dysfunction. Patients under the age of fifteen, pregnant or lactating women, as well as those suffering from Meniere's syndrome, otosclerosis, dizziness, and tinnitus were excluded from the study. Patients with symptoms for less than three months were also excluded.
All patients had scheduled appointments with an otolaryngologist who performed an audiology examination. Among the examinations performed were audiometric and impedance testing, rhinomanometry, otovideoendoscopy, the Italian nose obstruction symptom evaluation (I-NOSE) scale, the Sino-Nasal Outcome Test-22 (SNOT-22) questionnaire, and the Eustachian Tube Dysfunction Questionnaire-7 (ETDQ-7). All of the patients showed symptoms associated with Eustachian tube dysfunction, as confirmed by the aforementioned examinations. Before minimally invasive treatment, CT scans were performed on patients' Eustachian tubes in order to assess cartilage length, bone structure, and the angle of the tube. Pure-tone audiometry was performed in accordance with international standards (ISO 8253-1). We obtained the pure tone average of four frequency thresholds at 500, 1000, 2000, and 4000 Hz.
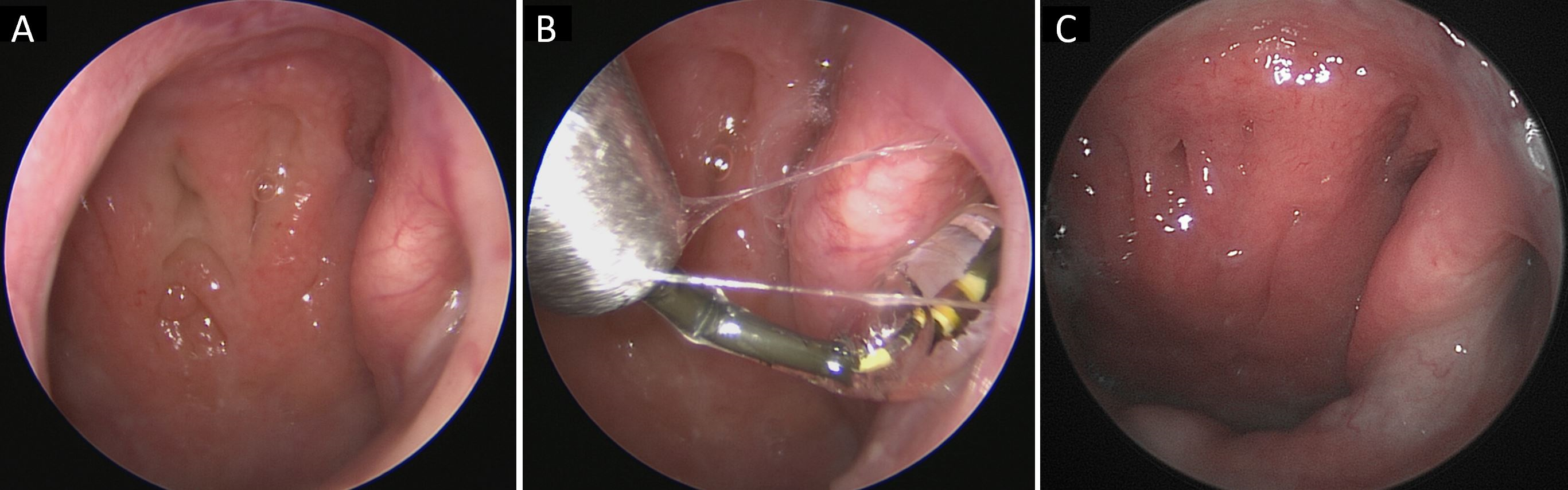
A comprehensive treatment program was administered to ensure maximum effectiveness. The patients all underwent functional endoscopic sinus surgery, turbinoplasty involving removal of the middle and lower turbinates, tubal ostium shrinkage, and shockwave tubodilation technique. The procedure was performed under general anesthesia. This minimally invasive procedure involved the use of an optical fiber of 3 millimeters in diameter (Karl Storz, Tuttlingen, Germany) and shockwave tubodilation on the ipsilateral Eustachian tube. A shockwave intravascular lithotripsy system was used to perform the shockwave tubodilation technique [17]. In order to prevent damage to the mucosa of the Eustachian tube, the intravascular lithotripsy balloon was introduced within an Eicken smooth guide. After entering, the balloon was inflated to a pressure of 4 atmospheres. Two cycles of 10 shockwave pulses were delivered, and each cycle lasted 10 seconds. We allowed the balloon to remain inside the tube for an additional 40 seconds at 4 atm before removing it (Figure 1). The procedure was then repeated on the contralateral Eustachian tube. The interventions were performed at the Casa di Cura Santo Volto Hospital in Rome following approval by an institutional review board.
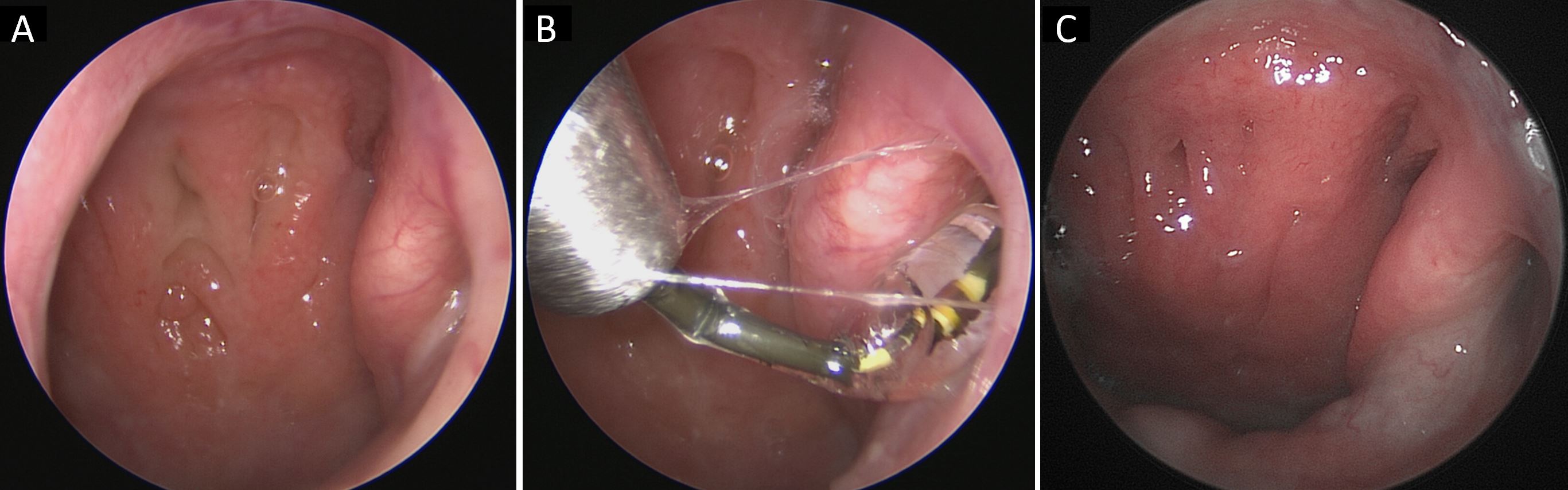
Figure 1. Endoscopic view of the shockwave tubodilation technique. (A) Preoperative view of the obstructive Eustachian tube. (B) Shockwave tubodilation. (C) The appearance of the Eustachian tube after 12 weeks of surgery.
The patients that participated in the study ranged in age from 35 to 70 years old. A follow-up examination was performed at 2 weeks and 4 weeks postoperatively on the patients (Table 1). During the audiometer examination before surgery, 9 out of the 10 patients (90%) had abnormal results, but only 5 of the 10 patients (50%) had abnormal results 2 weeks after surgery, and 2 out of 10 patients (20%) had abnormal results 4 weeks following surgery. Among the 10 patients, 9 (90%) patients had abnormal results on their impedance tests prior to surgery, but only 5 (50%) patients had abnormal results 2 weeks after surgery, and 2 (20%) patients had abnormal results 4 weeks after surgery. There were abnormal rhinomanometer results in 9 out of 10 patients (90%) prior to surgery, but only 4 of 10 patients (40%) had abnormal rhinomanometer results 2 weeks following surgery, and only 1 (10%) patient had abnormal rhinomanometer results 4 weeks after surgery.
The mean score of the SNOT-22 questionare before surgery was 48, and the mean score was 4 and 0 respectively after surgery at 2 and 4 weeks postoperatively. In the I-NOSE questionnaire, the average value before surgery was 17, and the average score after surgery at 2 and 4 weeks postoperatively was 0 and 0. In the EDTQ-7 questionnaire, the mean score prior to surgery was 33, and 2 and 4 weeks after surgery the mean scores were 7 and 7, respectively.
In our study, there were no complications observed. This shockwave did not cause injury to the mucosa of the tubal ostium, nor did the shockwave damage the neighboring organs. A nosebleed was not experienced as a result of this shockwave.
This novel shockwave tubodilation technique was specifically developed to treat Eustachian tube dysfunction in a safe, fast, minimally invasive manner. This approach was developed based on an established shockwave intravascular lithotripsy system. A recent study found that shockwaves play an important role in the regulation of macrophage functions in wound healing [16]. The immunomodulation represents an underappreciated effect of clinically applied shock waves, which could be exploited to treat other macrophage-associated conditions, such as Eustachian tube dysfunction [15,16]. The results of this study provide support for the use of shockwave tubodilation technique on patients suffering from disorders related to Eustachian tube dysfunction [16].
The shockwave tubodilation technique offers the advantage of a shorter procedure duration even in the most difficult cases (1 minute in total), allowing for a more effective procedure to be performed in a shorter time frame. In addition, the shockwave tubodilation technique permits a quicker execution of the surgical technique when compared to traditional balloon dilation (60 seconds as opposed to 120 seconds).
The present study is the first of its kind that demonstrates the use of shockwaves on the Eustachian tube. Furthermore, it summarizes the results of ten cases of refractory otitis media with effusion associated with Eustachian dysfunction. In addition, the insertion of a ventilation tube into the eardrum to treat Eustachian tube dysfunction often results in tympanic scarring and unhealing eardrum perforations, which require hospitalization and the associated expenses. A major benefit of the shockwave tubodilation technique is that it does not require hospitalization. In this way, the patient can return to normal life on the same day as the operation, resulting in an extremely low level of absenteeism from work.
This study emphasizes the importance of evaluating both subjective and objective data following shockwave tubodilation technique. In order to reach a conclusion regarding the effectiveness of this specific treatment modality, further investigation is required. In addition, a large-scale study will be required to determine the reliability and safety of this procedure. Furthermore, this technology has yet to be established whether it will have a long-term clinical impact. This study has another limitation in that the number of cases is relatively small. Currently, we are extending the number of cases so that the results of the study can be precisely validated. There is also the issue of the device's cost, which hopefully can be reduced in the future. It is also important to note that even though all patients had completely recovered from symptoms of tubal dysfunction approximately three months after surgery, they all underwent functional endoscopic sinus surgery, turbinoplasty, tubal ostium shrinkage, and shockwave tubodilation. Therefore, it may be challenging to determine the true therapeutic effects of each surgical procedure. It may be necessary to conduct further studies in order to clarify this issue.
The shockwave tubodilation technique has been demonstrated to be effective in treating patients suffering from otitis media with effusion resulting from Eustachian tube dysfunction. The preliminary results have motivated us to extend the number of cases studied and conduct further research to determine whether the positive short-term outcomes of shockwave tubodilation technique may have led to long-term improvements.
Received date: November 09, 2021
Accepted date: January 05, 2022
Published date: February 28, 2022
The study is in accordance with the ethical standards of the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
This research has received no specific grant from any funding agency either in the public, commercial, or not-for-profit sectors.
There are no conflicts of interest declared by either the authors or the contributors of this article, which is their intellectual property.
It is pertinent to note that all opinions and statements made by the author(s) throughout this article are solely those of the author(s). They may not be representative of those of their affiliated organizations, the publishing house, editors, or other reviewers since they are the opinions and statements of the author(s) alone. The publisher does not guarantee or endorse any statements made by the manufacturer of any product mentioned in this article or the author's evaluation.
© 2022 The Author(s). This is an open-access article distributed under the terms of the Creative Commons Attribution 4.0 International License (CC-BY). In accordance with accepted academic practice, anyone may use, distribute, or reproduce this material, so long as the original author(s), the copyright holder(s), and the original publication of this journal are credited, and this publication is cited as the original. To the extent permitted by these terms and conditions of license, this material may not be compiled, distributed, or reproduced in any manner that is inconsistent with those terms and conditions.
A comprehensive understanding of the mechanism underlying vertigo is essential to elucidate the reciprocal causal relationship between laryn-gopharyngeal reflux and Eustachian tube obstruction.
Authors present two cases of dilatory Eustachian tube dysfunction caused by localized nasopharyngeal amyloidosis.
Authors present two cases of dilatory Eustachian tube dysfunction caused by localized nasopharyngeal amyloidosis.
The clinical significance of otitis media with effusion (OME), a complication associated with cleft lip/palate (CLP), is often overlooked in children. The author reviews the pathogenesis, clinical manifestations, and diagnoses of OME in children with CLP as well as the controversies surrounding treatment. He also provides a flowchart to guide the management of OME in children with CLP.
Di Rienzo Businco L, Pavaci S, Tortorella F. First report on shockwave tubodilation technique for Eustachian tube dysfunction. Arch Otorhinolaryngol Head Neck Surg 2022;6(1):4. https://doi.org/10.24983/scitemed.aohns.2022.00157