Objective: Microsurgery is an advanced surgical procedure which requires advanced skills and techniques. These skills and techniques can generally be learned, practiced, replicated, improved, and evaluated. The majority of models and training pads in microsurgery have been reported to be used in fields other than spine surgery. This study was designed to develop and evaluate a portable, reusable and economical microsurgery training model that can be used by spinal surgery trainees in order to learn basic skills and gain self-confidence within microsurgery.
Methods: We developed a simulation training program that was implemented at a spine surgery center in Mexico City. The study involved six residents from the center who volunteered to participate in a 5-day assessment before and after the implementation of our model. The students were instructed in a simulation of laminectomy and repair of the dura mater during their training. A 5-point Likert scale was used to determine the level of confidence of surgical trainees in performing laminectomy and dural repair using microsurgical technique (where 1 represents no confidence and 5 represents excellent confidence). Five experienced spinal surgeons evaluated trainees blindly using the Stanford Microsurgery and Resident Training (SMaRT) scale. There are nine categories in the SMaRT scale, each of which is graded on a 5-point Likert scale. Results from quantitative and categorical data were analyzed using Student's t-tests and two-sample tests of proportions.
Results: The residents evaluated were aged 31 ± 1.4 years. None of them had previously undergone microsurgery. Training took an average of 4.75 hours. All participants were unable to complete the exercise before the training model, but all completed it afterward, with a mean time of 22.3 minutes. The median self-confidence score of surgical trainees increased from 1.5 to 3.5 after the exercise (P = 0.026). After the dural repair exercise, the participants completed an average of 5 ± 0 stitches, which was significantly higher than their initial average of 0.5 ± 0.8 stitches (P <0.001). The SMaRT score increased from 13.7 to 28.3 after training (P = 0.0001).
Conclusion: Training with simulated models can standardize skills and increase confidence. With the training model proposed in the study, participants are able to develop the skills necessary to perform spine microsurgery. A further study is needed to establish the validity of our training model for spine microsurgery.
Microsurgery has become a significant component of several surgical specialties [1]. As a complex surgical procedure, microsurgery requires highly advanced skills that can be taught, reproduced, improved, and assessed [2,3]. A traditional approach to microsurgery training is based on the Halsted model, which emphasizes the need for residents to repeatedly undergo surgery under the supervision of experienced surgeons to become proficient in performing operations [1,4]. However, the ethical concern for patient safety along with the reduction in surgical procedures resulting from the COVID-19 pandemic results in an insufficient number of trainees being exposed to surgical procedures. The training and attainment of skills in both basic and advanced surgical techniques are therefore highly limited [5-8].
The need for microsurgical skill development, teaching, and maintenance has compelled surgical training centers to implement innovative training strategies that provide a secure, controlled, and effective learning environment. A wide variety of training models have been developed, but most of them have examined areas other than spine surgery, for example, gauze exercises to improve revascularization techniques, mannequin heads with small balloons to improve deep microsurgical skills in neurosurgery, silastic tubes and chicken wings arteries for performing anastomosis, and the chicken egg and skull model to support endoscopy using the endonasal transsphenoidal approach [9-11].
Therefore, the authors developed a simulation training model in which spinal surgical trainees can acquire and enhance basic microsurgery skills during the training process, as well as enhance their self-confidence as they take part in the training process. This study aims to evaluate the effectiveness of this model for training in spinal microsurgery.
During the study, we evaluated residents from a spine surgery center in Mexico City. In the exercise, the participant was required to complete a laminectomy with a high-speed burr and repair the dura with five 10-0 nylon stitches within a time limit of 30 minutes. A performance evaluation of the participant was conducted prior to and five days after the exercise.
We used a 5-point Likert scale to assess the level of confidence among surgical trainees regarding performing laminectomy and dural repair using microsurgical technique (with 1 being no confidence and 5 being an excellent level of confidence). The study defined previous surgical experience as performing at least five microsurgical procedures as the primary surgeon (i.e., performing more than 80% of all procedures) [12].
The video recordings of the exercises were taken and examined by five experienced spine surgeons who are professors at the Spine Surgery Course and members of the Mexican Association of Spine Surgeons. The Stanford Microsurgery and Resident Training (SMaRT) rating scale was used to evaluate the performance of the participants in this study [13]. Based on the SMaRT scale, nine categories were evaluated on a Likert scale of 1 to 5. These categories include instrument handling, respect for tissue, efficiency, suture handling, suturing technique, quality of knot, final product, operation flow and overall performance. We blinded the evaluators by concealing information about both the participants and the timing of the study (before or after the training).
Step-by-step Instructions for Each Exercise
There were five basic exercises and a final exercise performed on a 30 x 30 x 7 cm foam pad with a stereomicroscope (Zeigen™, Mexico City). There was a 10x magnification on the objective, and the working distance between the objective and the objective lens was 30 cm (12 inches). Figure 1 shows the microscope, the instruments, and basic exercises placed in the proper arrangement, as they should be used. The final activity served as an evaluation exercise because it allowed the skills developed in the previous exercises to be incorporated into the final one.

Figure 1. Arrangement of the microscope, instruments, and basic exercises. (A) Microscope and microsurgical training pad equipped with basic microsurgical instruments, including micro scissors, dissection forceps, and a microsurgical needle holder. (B) A single training pad can accommodate six different exercises, allowing trainees to practice with both hands to simulate the patient's back, and to practice fine movements only using the wrist and fingers to reduce physiological tremor.
Round the clock
We arranged sewing needles of normal size in a circular pattern to form a circle with a diameter of 3.4 cm. The 10-0 suture was tied at 12:00 o'clock as the starting point and passed through the sewing needle holes clockwise and counterclockwise (Figure 2A) [13].
Three towers
There was a cubic space measuring 2 x 2 x 4 cm, containing two parallel needles arranged vertically and a third needle arranged horizontally. Ten acrylic beads were placed on one of the needles. During the training, the trainees were required to move the 10 beads from one needle to another (Figure 2B).
Erasing letters
In a cardboard card printed in Arial 12 font and measuring 9 x 5 cm, the caption reads "Mexico City Spine Clinic: Microsurgical training pad". The trainee had to use a needle to erase the letters without damaging the cardboard that surrounds the letters (Figure 2C) [14].
Bubble wrap cutting and suturing
The trainee was presented with a cardboard card measuring 9 x 5 cm, enclosed with bubble wrap measuring 1 cm in diameter. The trainee was instructed to cut the bubble wrap with micro scissors and suture it with simple (interrupted), continuous, or anchored stitches (Figures 2D-E) [15].
Eggshell drilling
An eggshell was positioned in a 4 x 4 x 6 cm space. The image of a vertebra was then drawn on the eggshell. The eggshell should be drilled using a high-speed microsurgical drill (32,000 revolutions per minute) along the edges of the vertebra on the eggshell without rupturing the membrane (Figure 2F).
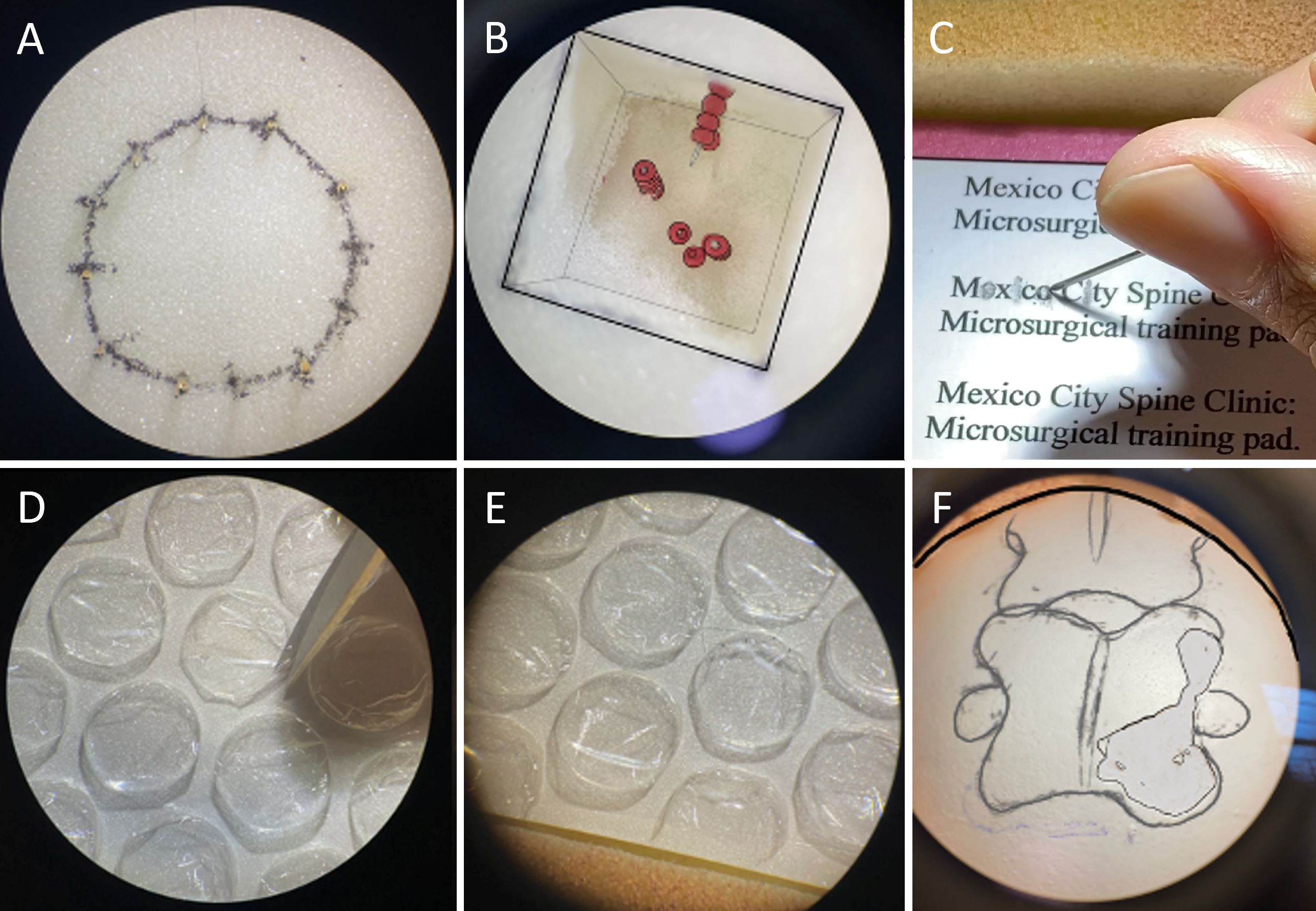
Figure 2. A step-by-step description of each exercise. (A) Round the clock. The needles are arranged in a circular pattern to create a circle with 3.4 cm (1.33 inches) diameter. In this procedure, the first suture is tied at 12:00 o'clock as the starting point, followed by the sutures passing through the sewing needle holes clockwise and counterclockwise. (B) Three towers. In a cubic space measuring 2 x 2 x 4 cm, two parallel needles are arranged vertically, and a third needle is arranged horizontally. A total of ten acrylic beads are placed on one needle. Participants in the training session are required to move ten beads from one needle to another. (C) Erasing the letters. The card measures 9 x 5 cm and has a caption in Arial 12 that reads "Mexico City Spine Clinic: Microsurgical training pad". In this exercise, the trainee is required to erase the letters using a needle without damaging the cardboard that surrounds them. (D) Bubble wrap cutting. Each trainee receives a cardboard card measuring 9 x 5 cm, enclosed in bubble wrap measuring 1 cm in diameter. The trainee is required to cut the bubble wrap using micro scissors. (E) Bubble wrap suturing. The trainee is then instructed to suture the bubble wrap either with simple (interrupted), continuous, or anchored stitches after cutting it. (F) Eggshell drilling. During the process, a shelled egg is placed in a space that measures 4 x 4 x 6 cm. An image of a vertebra is then drawn on the eggshell. Using a high-speed microsurgical drill (32,000 revolutions per minute), the edge of the vertebra on the eggshell is drilled through without causing any damage to the membrane.
Final activity
This step involved the simulation of laminectomy and duraplasty in order to evaluate the performance of incorporated skills which were developed in the earlier exercises. An anatomical model of vertebrae was made of polyvinyl chloride with a silicone pad in the middle. The laminectomy was simulated using a microsurgical drill, followed by simulated dura repairs completed with 10-0 nylon interrupted stitches (Figure 3).
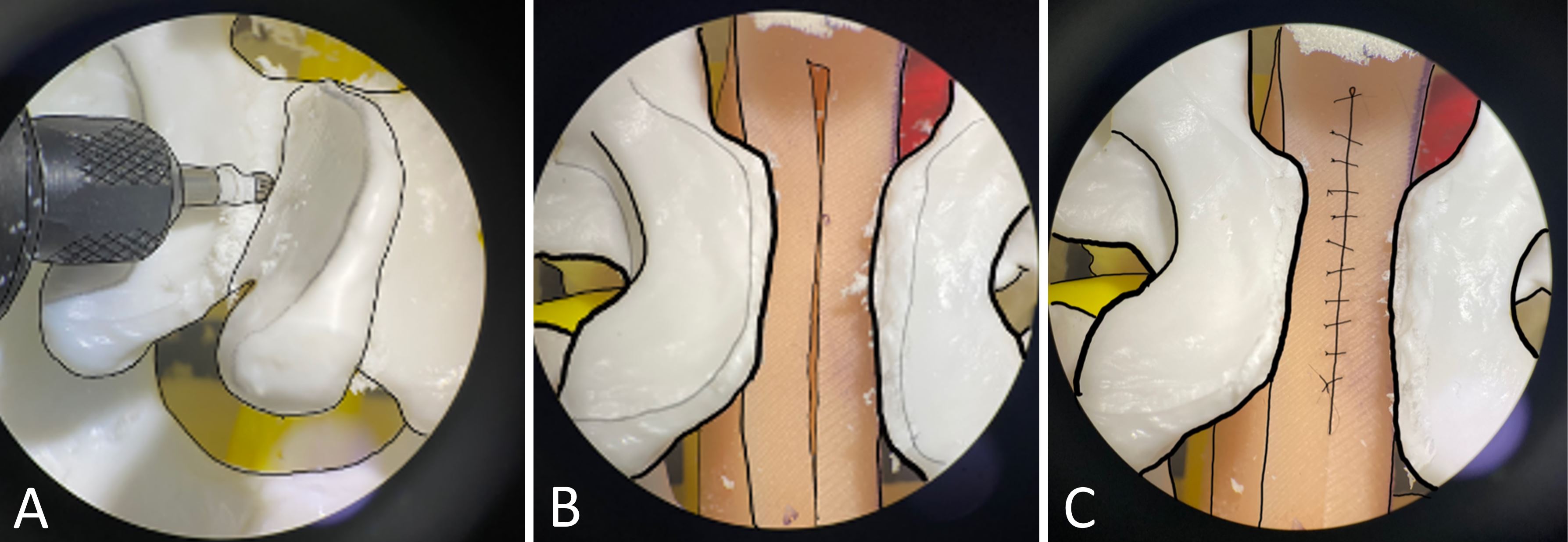
Figure 3. A final activity is used to assess all the earlier skills. (A) With the assistance of a microsurgical drill, a simulated laminectomy is performed. (B) Simulation of laminectomy with silicone pad exposure. (C) Simulated dura repair with interrupted stitches.
Statistical Analysis
We reported parametric quantitative variables with the means and standard deviations, and categorical variables with the frequency and percentage. Non-parametric, quantitative variables were expressed as medians and interquartile ranges. The participants were categorized based on their age, previous training experience, exercise duration, and training hours. Students' t-tests were used to analyze quantitative data, and an immediate form of the two-samples test of proportions was used to analyze categorical data. A Wilcoxon Signed Rank test was used to compare the magnitude of the quantitative variables before and after the intervention. The interobserver agreement was measured with Cohen's kappa. Statistical analyses were conducted with Stata 14 (Stata Corporation, TX 77845, USA).
The average age of the six residents evaluated was 31 ± 1.4 years. None of these residents had any previous experience performing microsurgery. An average of 4.75 ± 0.9 hours was devoted to the training program by each participant.
After the training model was implemented, 100% of the participants completed the exercise within their maximum time limit of 30 minutes, compared to 0% of participants before the training model, with a mean time of 22.3 minutes.
According to the self-confidence scale used for surgical trainees, a median rating of 1.5 was reported before the exercise; however, after the exercise the median rating was 3.5 (P = 0.026).
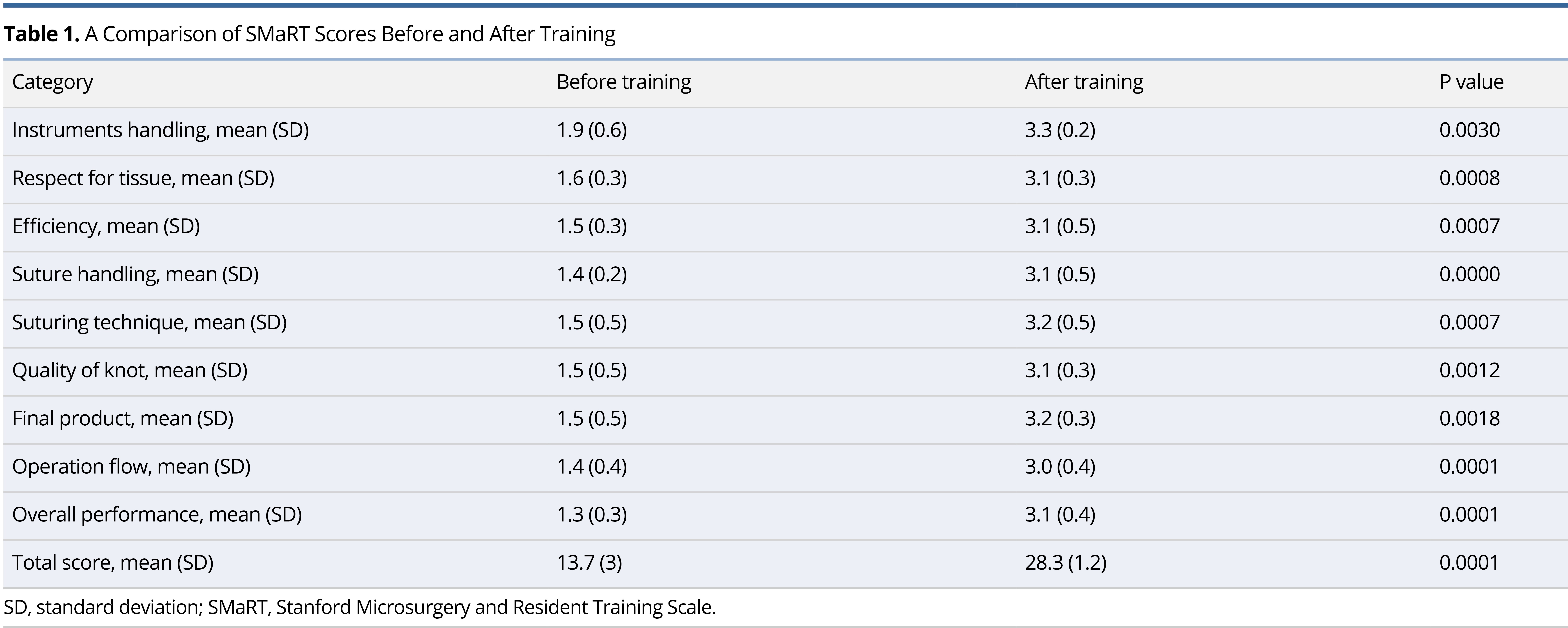
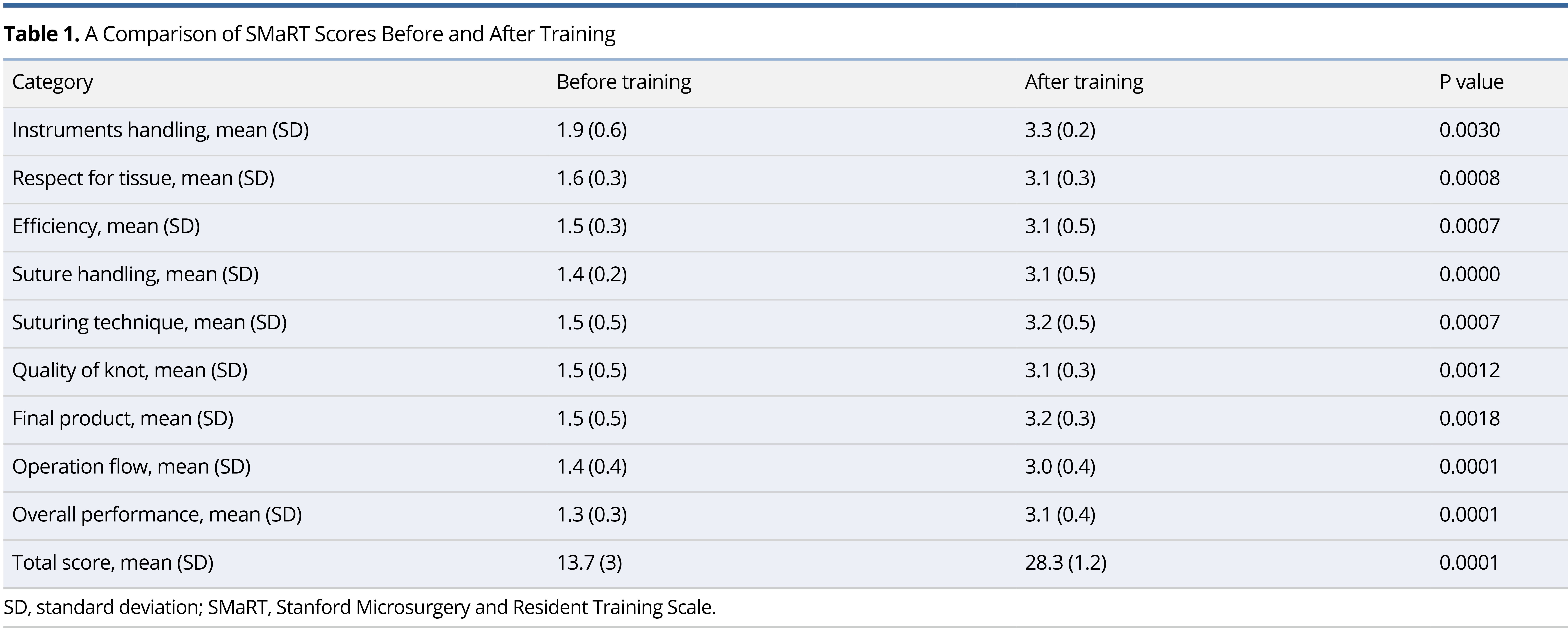
As a result of the dural repair exercise, the participants completed an average of 5 ± 0 stitches, which is significantly higher than the average of 0.5 ± 0.8 stitches they completed before the exercise (P <0.001). According to Table 1, the SMaRT scores improved from 13.7 to 28.3 before and after the training process (P = 0.0001).
Microsurgery is an extremely specialized field that requires a high level of skill and knowledge. These skills include microdissection, handling instruments and tissues, adaptation to microscopic vision, and the coordinated use of the hand and eye. A wide variety of training methods may be used in microsurgery training programs, including animals, virtual models, and artificial models [1,9]. These types of programs provide trainees with the opportunity to become familiar with basic surgical techniques in a laboratory environment before applying that knowledge to actual patients in the operating room [2].
In this study, we seek to design a training program through a simulation training model, which would enable spinal surgery trainees to acquire early experience with microsurgery as well as improve their confidence. Following completion of the training, the participants demonstrated significant improvements in the time required to complete the exercise, the number of knots successfully tied, and the items assessed on SMaRT scales, as well as the participants' perceptions of their confidence as a result of the training. In the present study, a 5-day microsurgery training program was implemented based on previous studies [2-4,9,12-15]. Nevertheless, there has not yet been a consensus regarding the ideal duration of a microsurgery course.
Due to the ethical issues associated with animal models, and the fact that virtual models are currently expensive and not widely accessible, artificial models are highly appealing since they do not have these disadvantages [1,2,10]. In one study, the use of animal models was reduced on the first day of training when an artificial model was used, while on the third day of training, the number of patent anastomoses increased [2]. In the present study, an innovative training pad was developed which has the potential of being widely available as well as affordable. In addition, a key benefit of this model is that it features a sponge surface that allows us to include six different exercises (Figure 1). It is therefore possible for trainees to place both hands on the pad to simulate a patient's back and to reproduce fine movements using only their wrists and fingers, thereby decreasing physiological tremor [16].
Handling sutures is one of the first challenges trainees encounter in microsurgery. Considering this issue, it has been recommended that the first exercises be focused on handling instruments and sutures (under control, in single passes, never grasp the needle tip, pull the needle out on a curve). Our simulation model began with a validated exercise called "round the clock", which enables trainees to become familiar with the use of micro-sutures [17]. The "three towers" exercise was specifically designed to improve movement in a restricted space with varying depths and directions [16]. In the next exercise, trainees erased letters, which was intended to teach them how to handle tissue in a careful, appropriate, and safe manner while causing the least amount of damage to it [14]. A bubble wrap suturing procedure involved cutting, dissecting, and suturing. It was initially intended to simulate arachnoids and blood vessels [10,15]. The model used egg shield drilling as a prelude to the last activity, which was simulation of laminectomy and duraplasty. Egg shield drilling was initially described as a way to simulate the delicate membrane in the transsphenoidal approach [11,16].
Study Limitations
It has been argued that trainee performance should be monitored immediately after training as well as after a certain period of time, in order to measure retention over time [12]. The main reason for this is that practice alternating with periods of rest (distributed practice) creates a constructive environment in which skills are acquired as well as retained more effectively than practice delivered continuously (massed practice). This study, however, did not examine the effects of training immediately following training, which constituted one of its limitations. A further limitation was that only a pre- and post-evaluation was conducted following the five consecutive days of practice (mass practice), thus the gradual efficacy of the training could not be measured.
Models may be validated in a variety of ways, including content validity (the ability to measure a specific skill), construct validity (the test is designed to assess the skill level for which it was designed), concurrent validity (the model produces the same results as the gold standard) and predictive validity (the model can produce the same results in the operating room) [1,9,13]. In this study, a blind evaluation was presented with both content and construct validity. However, the study was unable to assess concurrent validity because there has not been a gold standard for microsurgical practice in the field of spine surgery. There is also a need for further studies to assess the retention of acquired skills and the predictive validity of the results [1,4,9].
The proposed training model provides a unique opportunity for trainees to acquire and develop advanced skills related to spine microsurgery, which are required in the clinical practice of the specialty. A training program with artificial models allows for the standardization of skills and the improvement of confidence through a consistent training approach. Further research is necessary to develop new and validated training models for spine microsurgery.
Received date: January 05, 2022
Accepted date: April 01, 2022
Published date: June 01, 2022
Oscar Josue Montes Aguilar (https://orcid.org/0000-0002-5500-3052).
Our team wishes to thank the residents and professors from the Dr. Manuel Dufoo Olvera Spine Clinic of the Health Department of Mexico City for their participation in the evaluation. We appreciate their generous support and participation. Their efforts were imperative to the success of this work.
Neither the study nor its findings have been presented at any meetings or conferences.
The study is in accordance with the ethical standards of the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
This research has received no specific grant from any funding agency either in the public, commercial, or not-for-profit sectors.
There are no conflicts of interest declared by either the authors or the contributors of this article, which is their intellectual property.
It should be noted that the opinions and statements expressed in this article are those of the respective author(s) and are not to be regarded as factual statements. These opinions and statements may not represent the views of their affiliated organizations, the publishing house, the editors, or any other reviewers since these are the sole opinion and statement of the author(s). The publisher does not guarantee or endorse any of the statements that are made by the manufacturer of any product discussed in this article, or any statements that are made by the author(s) in relation to the mentioned product.
© 2022 The Author(s). This is an open-access article distributed under the terms of the Creative Commons Attribution 4.0 International License (CC-BY). In accordance with accepted academic practice, anyone may use, distribute, or reproduce this material, so long as the original author(s), the copyright holder(s), and the original publication of this journal are credited, and this publication is cited as the original. To the extent permitted by these terms and conditions of license, this material may not be compiled, distributed, or reproduced in any manner that is inconsistent with those terms and conditions.
The author reframes review articles as evidence infrastructure that updates clinical consensus and identifies research gaps. The author argues that narrative reviews integrate findings across biological scales and translate molecular data into clinically meaningful explanations of disease behavior. Using cholesteatoma, the author illustrates how molecular evidence can recast invasiveness and recurrence into a mechanistic model that also motivates the pursuit of nonsurgical therapies. The author contrasts this interpretive role with systematic reviews, which function as reproducible decision chains grounded in transparent, verifiable methodology. Finally, the author cautions that AI assisted automation can propagate error unless it is governed by expert oversight within a human in the loop model that preserves auditable decision chains.
The communication among international microsurgeons have switched from one direction (from paper, textbook) to multiway interactions through the internet. The authors believe the online platform will play an immensely important role in the learning and development in the field of microsurgery.
Traditionally, suturing techniques have been the mainstay for microvascular anastomoses, but owing to its technical difficulty and labour intensity, considerable work has gone into the development of sutureless microvascular anastomoses. In this review, the authors take a brief look at the developments of this technology through the years, with a focus on the more recent developments of laser-assisted vascular anastomoses, the unilink system, vascular closure staples, tissue adhesives, and magnets. Their working principles, with what has been found concerning their advantages and disadvantages are discussed.
Prof. Koushima, president of World Society for Reconstructive Microsurgery, proposes an innovative concept and technique of the multi-stage ‘Orochi’ combined flaps (sequential flaps in parallel). The technique opens a new vista in reconstructive microsurgery.
The video presents a useful technique for microvascular anastomosis in reconstructive surgery of the head and neck. It is advantageous to use this series of sutures when working with limited space, weak vessels (vessels irradiated, or with atheroclastic plaques), suturing in tension, or suturing smaller vessels (less than 0.8 cm in diameter).
Authors discuss a silicone tube that provides structural support to vessels throughout the entire precarious suturing process. This modification of the conventional microvascular anastomosis technique may facilitate initial skill acquisition using the rat model.
PEDs can be used as alternative means of magnification in microsurgery training considering that they are superior to surgical loupes in magnification, FOV and WD ranges, allowing greater operational versatility in microsurgical maneuvers, its behavior being closer to that of surgical microscopes in some optical characteristics. These devices have a lower cost than microscopes and some brands of surgical loupes, greater accessibility in the market and innovation plasticity through technological and physical applications and accessories with respect to classical magnification devices. Although PEDs own advanced technological features such as high-quality cameras and electronic loupes applications to improve the visualizations, it is important to continue the development of better technological applications and accessories for microsurgical practice, and additionally, it is important to produce evidence of its application at surgery room.
Avulsion injuries and replantation of the upper arm are particularly challenging in the field of traumatic microsurgery. At present, the functional recovery of the avulsion injuries upper arm after the replantation is generally not ideal enough, and there is no guideline for the surgeries. The aim of this study was to analyze the causes of failure of the upper arm replantation for avulsion injuries, summarize the upper arm replantation’s indications, and improve the replantation methods.
The supraclavicular flap has gained popularity in recent years as a reliable and easily harvested flap with occasional anatomical variations in the course of the pedicle. The study shows how the determination of the dominant pedicle may be aided with indocyanine green angiography. Additionally, the authors demonstrate how they convert a supraclavicular flap to a free flap if the dominant pedicle is unfavorable to a pedicled flap design.
The implications of rebound heparin hypercoagulability following cessation of therapy in microsurgery is unreported. In this article the authors report two cases of late digit circulatory compromise shortly after withdrawal of heparin therapy. The authors also propose potential consideration for changes in perioperative anticoagulation practice to reduce this risk.
The loupe plays a critical role in the microsurgeon's arsenal, helping to provide intricate details. In the absence of adequate subcutaneous fat, the prismatic lens of the spectacle model may exert enormous pressure on the delicate skin of the nasal bone. By developing a soft nasal support, the author has incorporated the principle of offloading into an elegant, simple yet brilliant innovation. A simple procedure such as this could prove invaluable for microsurgeons who suffer from nasal discoloration or pain as a result of prolonged use of prismatic loupes. With this technique, 42% of the pressure applied to the nose is reduced.
An examination of plastic surgery residents' experiences with microsurgery in Latin American countries was conducted in a cross-sectional study with 129 microsurgeons. The project also identifies ways to increase the number of trained microsurgeons in the region. The authors claim that there are few resident plastic surgeons in Latin America who are capable of attaining the level of experience necessary to function as independent microsurgeons. It is believed that international microsurgical fellowships would be an effective strategy for improving the situation.
This retrospective study on the keystone design perforator island flap (KDPIF) reconstruction offers valuable insights and compelling reasons for readers to engage with the article. By sharing clinical experience and reporting outcomes, the study provides evidence of the efficacy and safety profile of KDPIF as a reconstructive technique for soft tissue defects. The findings highlight the versatility, simplicity, and favorable outcomes associated with KDPIF, making it an essential read for plastic surgeons and researchers in the field. Surgeons worldwide have shown substantial interest in KDPIF, and this study contributes to the expanding knowledge base, reinforcing its clinical significance. Moreover, the study's comprehensive analysis of various parameters, including flap survival rate, complications, donor site morbidity, and scar assessment, enhances the understanding of the procedure's outcomes and potential benefits. The insights garnered from this research not only validate the widespread adoption of KDPIF but also provide valuable guidance for optimizing soft tissue reconstruction in diverse clinical scenarios. For readers seeking to explore innovative reconstructive techniques and improve patient outcomes, this article offers valuable knowledge and practical insights.
This comprehensive review article presents a profound exploration of critical facets within the realm of microsurgery, challenging existing paradigms. Through meticulous examination, the authors illuminate the intricate world of microangiosomes, dissection planes, and the clinical relevance of anatomical structures. Central to this discourse is an exhaustive comparative analysis of dermal plexus flaps, meticulously dissecting the viability and potential grafting applications of subdermal versus deep-dermal plexi. Augmenting this intellectual voyage are detailed illustrations, guiding readers through the intricate microanatomy underlying skin and adjacent tissues. This synthesis of knowledge not only redefines existing microsurgical principles but also opens new frontiers. By unearthing novel perspectives on microangiosomes and dissection planes and by offering a comparative insight into dermal plexus flaps, this work reshapes the landscape of microsurgery. These elucidations, coupled with visual aids, equip practitioners with invaluable insights for practical integration, promising to propel the field of microsurgery to unprecedented heights.
This article presents a groundbreaking surgical approach for treating facial paralysis, focusing on the combination of the pronator quadratus muscle (PQM) and the radial forearm flap (RFF). It addresses the challenges in restoring facial functions and skin closure in paralysis cases. The study's novelty lies in its detailed examination of the PQM's vascular anatomy when combined with the RFF, a topic previously unexplored. Through meticulous dissections, it provides crucial anatomical insights essential for enhancing facial reanimation surgeries, offering significant benefits in medical practices related to facial reconstruction and nerve transfer techniques.
This article exemplifies a significant advancement in microsurgical techniques, highlighting the integration of robotic-assisted surgery into the deep inferior epigastric perforator (DIEP) flap procedure for breast reconstruction. It demonstrates how innovative robotic technology refines traditional methods, reducing the invasiveness of surgeries and potentially lessening postoperative complications like pain and herniation by minimizing the length of the fascial incision. This manuscript is pivotal for professionals in the medical field, especially those specializing in plastic surgery, as it provides a comprehensive overview of the operative techniques, benefits, and critical insights into successful implementation. Moreover, it underscores the importance of ongoing research and adaptation in surgical practices to enhance patient outcomes. The article serves as a must-read, not only for its immediate clinical implications but also for its role in setting the stage for future innovations in robotic-assisted microsurgery.
The groundbreaking study illuminates the complex mechanisms of nerve regeneration within fasciocutaneous flaps through meticulous neurohistological evaluation, setting a new benchmark in experimental microsurgery. It challenges existing paradigms by demonstrating the transformative potential of sensory neurorrhaphy in animal models, suggesting possible clinical applications. The data reveal a dynamic interplay of nerve recovery and degeneration, offering critical insights that could revolutionize trauma management and reconstructive techniques. By bridging experimental findings with hypothetical clinical scenarios, this article inspires continued innovation and research, aimed at enhancing the efficacy of flap surgeries in restoring function and sensation, thus profoundly impacting future therapeutic strategies.
This article presents the first comprehensive review of refractory chylous ascites associated with systemic lupus erythematosus, analyzing 19 cases to propose an evidence-based therapeutic framework. It introduces lymphatic bypass surgery as an effective option for this rare complication, overcoming the limitations of conventional treatment. By integrating mechanical drainage, immunomodulation, and lymphangiogenesis, this approach achieves rapid and sustained resolution of ascites. The findings offer a novel surgical strategy for autoimmune lymphatic disorders and prompt a re-evaluation of their complex pathophysiology. This study demonstrates how surgical innovation can succeed where traditional therapies fail, offering new hope in managing refractory autoimmune disease.
This case highlights the use of a bipedicled deep inferior epigastric perforator (DIEP) flap for reconstructing a massive 45 × 17 cm chest wall defect following bilateral mastectomy. By preserving abdominal musculature and utilizing preoperative computed tomographic angiography (CTA) for perforator mapping, the technique enabled tension-free bilateral microvascular anastomosis to the internal mammary arteries. The incorporation of submuscular mesh and minimal donor-site undermining maintained abdominal wall integrity. At six-month follow-up, no hernia or functional deficits were observed, and the patient reported high satisfaction on the BREAST-Q. This muscle-sparing strategy offers a viable alternative for large, midline-crossing chest wall defects where conventional flaps may be insufficient.
Motorcycle chain-induced fingertip amputations represent a reconstructive dead end, where severe crushing and contamination traditionally compel revision amputation. The authors dismantle this exclusion criterion, reporting an 83% salvage rate using a modified protocol of radical debridement, strategic skeletal shortening, and simplified single-vessel supermicrosurgery. By eschewing complex grafting for tension-free primary anastomosis, the authors successfully restored perfusion in ostensibly
The authors present a novel synthetic vascular model for microanastomosis training. This model is suitable for trainees with intermediate level of microsurgical skills, and useful as a bridging model between simple suturing exercise and in vivo rat vessel anastomosis during pre-clinical training.
The review article presents an expansive list of otolaryngology-specific surgical simulation training models as described in Otolaryngology literature as well as evaluates recent advances in simulation training in Otolaryngology.
The groundbreaking study illuminates the complex mechanisms of nerve regeneration within fasciocutaneous flaps through meticulous neurohistological evaluation, setting a new benchmark in experimental microsurgery. It challenges existing paradigms by demonstrating the transformative potential of sensory neurorrhaphy in animal models, suggesting possible clinical applications. The data reveal a dynamic interplay of nerve recovery and degeneration, offering critical insights that could revolutionize trauma management and reconstructive techniques. By bridging experimental findings with hypothetical clinical scenarios, this article inspires continued innovation and research, aimed at enhancing the efficacy of flap surgeries in restoring function and sensation, thus profoundly impacting future therapeutic strategies.
The review article presents an expansive list of otolaryngology-specific surgical simulation training models as described in Otolaryngology literature as well as evaluates recent advances in simulation training in Otolaryngology.
Montes Aguilar OJ, Alaniz Sida KK, Dufoo Olvera M, Collado Arce MGL, Ladewig Bernaldez GI, Oropeza Oropeza E, Gómez Flores G, Pérez Rios JJ, Zambrano AM, Ambrosio Vicente MDJ, Silva Chavez R, Ochoa González MV. An innovative model for microsurgical training at a spine surgery center in Mexico City. Int Microsurg J 2022;6(1):2. https://doi.org/10.24983/scitemed.imj.2022.00161